Adjustable Gastric Band
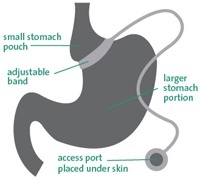
The LAGB is a common weight loss procedure which is minimally invasive, safe and with a fast recovery time.
Who Qualifies for a Gastric band?
You may be considered for a gastric band if you have a body mass index (BMI) that is greater than 40 (or greater than 35 if you experience a weight-related illness, such as type 2 diabetes, hypertension, sleep apnoea etc.) and you have tried other methods of weight loss, such as dieting, without long-term success. In certain circumstances patients with a lower BMI may be candidates.
The Surgery
The gastric band operation takes approximately 1-2 hours to complete and is performed via laparoscopic (keyhole) technique, under general anaesthesia. This involves making several small cuts (between 5 and 15mm in length) into the abdomen where the surgical instruments, including a camera, are inserted. The adjustable silicone ring (gastric band) is fitted around the top of the stomach where it is clipped into place. A fold of stomach is then sewn over the band to reduce the chance of the band slipping. The band is connected to a short tube and a port, which is secured under the skin in the abdomen, and which is used to add or remove fluid from the band in order to adjust its size. The port cannot be seen but can be felt when touching the skin overlying it.
How does the surgery assist in weight loss?
The gastric band assists patients to lose weight in two ways:
- By restricting the amount of food you can eat in one sitting. The band creates a small pouch at the top of the stomach that collects food after swallowing. It is smaller than a golf ball and can hold less than ½ a cup of food (whereas a typical stomach can hold up to 1 litre).
- By making you feel fuller faster and for longer. The action of each mouthful of food pushing against the band as it moves through it stimulates nearby nerves to send a message to your brain that the stomach is full.
It is important to remember that surgery is a tool to assist your weight loss journey and not the whole solution. It is vital that healthy lifestyle behaviours are practiced to get the best result from the procedure. Eating a variety of vegetables, fruits and lean proteins as well as limiting your intake of high-calorie foods such as sweets, fast food and sugary-drinks will maximise your weight loss after surgery. If eating behaviours are not adapted after surgery, weight loss will be slowed and limited and weight regain can occur in the future. More detailed information regarding healthy eating behaviours will be provided during your visit with the dietitian.
Expected weight loss
In general patients can lose up to half to two-thirds of their excess body weight. The time frame that this will take will vary from person to person, but an initial goal weight is usually reached approximately 18 to 24 months after surgery.
Regular adjustments to the size of the band are vital to its success. This is required to balance the restricting size of the stomach in order to achieve good weight loss whilist maintaining comfort, quality of life and minimising side effects. The band is required to be adjusted every 4-6 weeks for the first 12-18 months after placement. You must work with your doctor to get the balance right as BOTH too loose and too tight can reduce your weight loss. The adjustments are made without sedation or surgery, via an injection through the skin into the port that was put into place during band insertion. Adding more sterile salt water will further inflate the band (increasing restriction) and removing some water will deflate and loosen the band.
Advantages of a Gastric Banding
- This procedure does not require parts of the stomach to be removed or stapled as with other weight loss surgeries. Therefore nutrients, such as vitamins and minerals, are absorbed from food in the same way that they were prior to surgery, greatly lowering the risk of any nutrient deficiency.
- It is the safest weight loss procedure. It is the least invasive surgical weight loss option with no stomach stapling or intestinal rerouting required.
Disadvantages of a Gastric Banding
- The intensity of follow up. Frequent band adjustment appointments, especially in the first 12-months after surgery, are required to achieve optimal weight loss results.
- Weight loss is more variable between individuals and generally lower compared with more aggressive weight loss surgeries, such as the gastric sleeve or bypass.
- For safe and effective weight loss, substantial changes to diet and eating behaviours are necessary. It is important to take smaller mouthfuls, chew well and eat slowly.
Risks of the Gastric Banding
As with any surgical procedure, there are risks associated with the gastric banding operation. It is important to understand these risks before proceeding with the operation. The following is a list of potential risks that should be discussed in greater detail with your surgeon.
Possible Acute Complications
Possible immediate/short-term Complications
- Infection – which may require treatment with antibiotics and occasionally repeat operation.
- Damage to Organs – unintentional injury to the organs near the area of operation. This may require a repeat operation to repair the damaged organs.
- Blood Clots – such as deep vein thromboses (clots in the veins, usually of the legs) and pulmonary embolus (clots in the lungs).
- Pneumonia/ chest infection
Possible Long-Term Complications
There are some possible long-term surgical problems related to the gastric band itself:
- The band can slip (move too high or too low on the stomach).
- The band can erode (push through the stomach wall into the stomach cavity). This complication occurs in up to 1% of cases and can require surgical removal of the band.
- Gastric pouch dilatation, or oesophageal dilatation, can occur above the band as a result of regular over-eating. This result in the band being ineffective as the volume of food you can tolerate comfortably increases, leading to weight gain. A second (revision) surgery may be required to modify or improve the band position. If dilatation is recurrent or persistent, the band may need to be removed.
- Nutritional deficiencies. These are very rare after gastric banding and can be avoided or detected early by regular reviews with your dietitian. Management involves vitamin and mineral supplementation.
Pre-Operative Diet
After receiving your date for surgery, you will be advised to start a very low-calorie liquid meal replacement diet for approximately 14 days prior to the surgery. OptifastTM is the recommended meal replacement and is readily available from your local Chemist. The diet is intended to kick-start your weight loss prior to surgery, aiming to reduce the size of your liver to optimise the safety of the procedure. More detailed information will be provided to you during your appointment with the dietitian.
Post-Operative Care
Most patients stay in hospital 3-5 days after their surgery to ensure the safety and effectiveness of the gastric band. After the procedure your diet will consist of clear fluids (water, black tea, broth, juices). You will need to sip fluids slowly. Before going home you will have an x-ray to check the position of the band. Once correct positioning is confirmed you will be able to drink fluids freely for the remainder of your hospital stay. During the next 4-6 weeks, while your body heals, you will gradually increase the consistency and volume of food you eat. Further information, including a healthy dietary guidelines booklet, will be provided at your appointment with the dietitian.
Appointments Surgeon
Your first post-operative clinic visit will be arranged for 1-3 weeks after your surgery. At this appointment your surgical wounds will be assessed, and any other issues will be discussed.
Dietitian
The dietitian will phone you within the first week following surgery to review your food intake. Your first post-operative clinic visit with the dietitian will be at 3 to 6 weeks after your surgery and then every monthly for the first 6 months and 3 to 6 monthly for the first two years.



















