Yes! Have you ever wondered why when you are tired you want to eat more? Your body subconsciously wants you to consume more calories at the point of fatigue, as it is attempting to increase energy levels the only way it knows how when you are awake: by eating.
Absentminded calorie consumption is common when you are overworked and overtired. Not only that, but the appetite regulation hormones leptin and ghrelin go out of whack too. Ghrelin normally peaks before a meal to signal for hunger, whereas leptin reaches higher levels after a meal to alert the body it is full. However, several studies analysing patients undergoing sleep deprivation found that the complete opposite occurs! Ghrelin spikes up for longer periods of time throughout the day, preparing the body for a long night awake. Leptin levels drop, which means the brain doesn’t receive any satiety signals. This in turn causes us to consume more food, either by increasing our portion sizes or snacking when we’re not really hungry.
The sleep-cycle of the body is called its circadian rhythm. Different hormones and proteins work at different times of the day to help the body rest, wake, eat, sleep, and maintain energy. For example, the hormone melatonin increases at night when it is dark outside, signalling the body that it’s time to sleep. In the morning, exposure to natural light decreases melatonin levels and helps us wake up.
Just like all the other hormones floating around the body helping us function, leptin and ghrelin are disrupted when we do not sleep enough. Late nights also increase our energy requirements, as the body is pushing to stay awake for longer. Studies in the Sleep Medical Journal found that participants who were awake later and had restricted sleep ended up consuming more calories on those days than their normal sleep days.
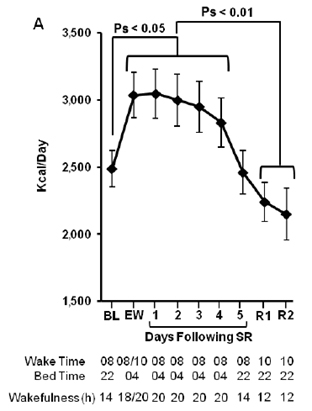
The graph to the left shows the amount of calories consumed, per day (on the vertical axis), during normal sleep and sleep restriction. Hours awake went from a relatively normal 14 hours to 18-20 hours when deprived of sleep (SR, sleep restriction). Fortunately, calorie consumption returned to normal when normal sleeping patterns resumed.
Source: Figure 2-A: Spaeth et al. (2013). Effects of Experimental Sleep Restriction on Weight Gain, Caloric Intake, and Meal Timing in Healthy Adults. Sleep, Vol. 36, No. 7.
All in all, it is crucial to support your weight-loss goals with healthy nutritious meals, regular exercise, consistent water intake and heading to bed at the same time every day. Fluctuations will occur, of course, as they do with any weight-loss journey, but doing your best to clock in at least 7-8 hours of sleep a night ensures that your body has been well rested to take on every day as it comes. It is important to think of weight loss surgery as a holistic lifestyle change, encompassing nutrition, exercise, mindset, stress management and adequate rest. Focusing on the combination of these factors is what will help set you up for long-term weight loss success!
We would love to hear your comments! Do you have a regular sleep routine or do you find it changes all the time? Let us know!
- By guess blogger, Alex Sherman
References
- Arble, D. M., Bass, J., Laposky, A. D., Vitaterna, M. H. and Turek, F. W. (2009), Circadian Timing of Food Intake Contributes to Weight Gain. Obesity, 17: 2100–2102
- Spaeth et al. (2013). Effects of Experimental Sleep Restriction on Weight Gain, Caloric Intake, and Meal Timing in Healthy Adults. Sleep, Vol. 36, No. 7.
- Chaput, J.P., Després, J.P., Bouchard, C., Tremblay, A. (2008). The Association Between Sleep Duration and Weight Gain in Adults: A 6-Year Prospective Study from the Quebec Family Study. Journal of Sleep Research, Vol 31: 517-523
- I also just found another article I didn’t really use, but I am going to read into it later, and I thought I would send it through if you can access and read it too, it looks pretty good!
- Schmid, S. M., Hallschmid, M., Jauch-Chara, J., Born, J., and Schultes, B. (2008), A single night of sleep deprivation increases ghrelin levels and feelings of hunger in normal-weight healthy men. Journal of Sleep Research, 17: 331–334




















