Sleeve Gastrectomy
Background
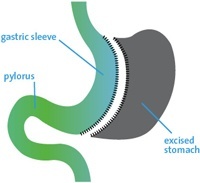
The sleeve gastrectomy, also known as the gastric sleeve resection or tube gastrectomy, involves the removal of approximately 90% of the stomach to reduce its food-holding capacity to around 100-200mL, resulting in significant weight loss.
Who Qualifies for A Sleeve Gastrectomy?
You may be considered for a sleeve gastrectomy if you have a body mass index (BMI) that is greater than 40 (or greater than 35 if you experience a weight-related illness, such as type 2 diabetes, hypertension, sleep apnoea etc.) and you have tried other methods of weight loss, such as dieting, without long-term success.
The Surgery
The sleeve gastrectomy procedure takes approximately 1-2 hours to complete and is performed with laparoscopic (keyhole) technique under general anaesthesia. This involves making small cuts (between 5 and 15mm in length) into the abdomen where the surgical instruments, including a camera, are inserted. The size of the stomach is reduced by stapling along its length (over a sizing device called a bougie) to form a long tube that looks similar to a banana. The excess stomach is removed from the body permanently.
How does the surgery assist in weight loss?
The sleeve gastrectomy assists patients to lose weight in two ways:
- Reducing the amount of food that can be eaten in one sitting. The volume of food the pouch can hold is greatly reduced, causing you to feel full from a small portion of food.
- Suppressing appetite. The stomach releases a hormone called ghrelin, which stimulates appetite. By decreasing the size of the stomach, the number of cells that release ghrelin is also reduced, therefore reducing appetite.
It is important to remember that surgery is a tool to assist your weight loss journey and not the whole solution. It is vital that healthy lifestyle behaviours are practiced to get the best result from your surgery. Eating a variety of vegetables, fruits and lean proteins as well as limiting your intake of high-calorie foods such as sweets, take-away and sugary-drinks will maximise your weight loss after surgery. If eating behaviours are not adapted after surgery, weight loss will be slowed and limited and weight regain can occur. More detailed information regarding healthy eating behaviours will be provided during your visit with the dietitian.
Expected weight loss
The sleeve gastrectomy results in significant weight reduction as well as long-term weight maintenance. Weight loss after a sleeve gastrectomy tends to be faster than other common operations. Most patients can expect to lose 25 to 35% of their total body weight over the first 12 months.
Advantages of a sleeve gastrectomy
- Great dietary quality of life. All foods can usually be tolerated, just in much smaller quantities.
- Typically rapid and reliable weight loss.
- No on-going adjustments, which are required with other procedures, such as the gastric band. However, regular follow up is still necessary to ensure your weight loss is appropriate and your food intake is nutritionally adequate.
Disadvantages of a sleeve gastrectomy
Disadvantages of the sleeve gastrectomy are generally related to the magnitude of the surgery:
- Complications, although rare, can be serious and should be discussed in detail with your surgeon.
- The sleeve gastrectomy is a relatively new operation. As a result, there is very little long-term data (data that follows patients beyond 10 years post-surgery). It is likely that the sleeve will dilate with time, reducing its effectiveness at limiting your food intake. Therefore developing healthy eating behaviours and lifestyle habits is vital to long-term success. All bariatric surgeries suffer in some way from this problem.
Risks of the Sleeve Gastrectomy
As with any surgical procedure, there are risks associated with the sleeve gastrectomy . It is important to understand these risks before proceeding with the operation. The following is a list of potential risks that should be discussed in greater detail with your surgeon.
Possible Acute Complications
Complications that can occur during the surgery or shortly after include:
- Bleeding – which can require blood transfusion and occasionally repeat operation. Bleeding occurs in roughly 1 in 200 patients.
- Leaks at the staple line- is a serious risk. It occurs in roughly 1 in 100 patients and can require a repeat surgery, often within the first few days after the original surgery. If a leak persists it can create a passage between the stomach and the skin or surgical wound (fistula) or cause persistent infections within the abdomen (abscesses). This complication can extend the length of stay in hospital to weeks or potentially months after surgery and can be a life-threatening problem.
- Infection – this may require treatment with antibiotics and occasionally repeat operation.
- Wound issues - this includes infections, haematomas (large bruises) and poor wound healing.
- Other extremely rare issues – as this surgery affects the function of the gut, some patients are unable to tolerate adequate intakes of food which can result in the requirement of long-term nutritional support via intravenous methods, called TPN (total parenteral nutrition).
- Damage to organs – unintentional injury to the organs near the area of operation. This may require a repeat operation to repair the damaged organs.
- Blood clots – such as deep vein thromboses (clots in the veins, usually of the legs) and pulmonary embolus (clots in the lungs).
- Pneumonia/ chest infection
Possible Long-Term Complications
- Adhesions (scar tissue) related to the gut. This can occur any time after the operation and can sometimes cause problems with the bowel getting stuck or twisted. It may require repeat surgery, sometimes in the emergency setting.
- Hernia formation at the site of wound closure. This may require repeat surgery, sometimes in the emergency setting.
- Increased chance of gastro-oesophageal reflux (heartburn). If reflux occurs post-operatively, some patients require acid-suppressing medication to relieve symptoms. This operation is best avoided in patients with severe symptoms of reflux prior to surgery.
- There are occasional issues related to malabsorption of micronutrients. These are usually easily managed with supplemental vitamins and minerals. Long-term monitoring with blood tests is required to detect these nutrient deficiencies.
Pre-Operative Diet
After receiving your date for surgery, you will be advised to start a very low-calorie liquid meal replacement diet for the 14 days prior to your surgery. OptifastTM is the recommended meal replacement and is readily available from your local Chemist. The diet is intended to kick-start your weight loss prior to surgery, with the aim of reducing the size of your liver to optimise the safety of the procedure. More detailed information will be provided to you during your appointment with the dietitian.
Post-Operative Care
Generally, patients will stay in hospital for 2-3 days following the procedure. After the procedure you will start drinking clear fluids only (water, black tea, broth, juices). These will need to be sipped slowly in small amounts. Once the size and function of the pouch is confirmed, you will be able to drink fluids freely for the remainder of your hospital stay. During the next 4-6 weeks, while your body heals, you will gradually increase the texture of food you eat. Further information, including a healthy dietary guidelines booklet, will be provided at your appointment with the dietitian.
Appointments
Surgeon
Your first post-operative clinic visit will be arranged for 2-4 weeks after your surgery. At this appointment your surgical wounds will be assessed, and any other issues will be discussed.
Dietitian
The dietitian will phone you within the first week following your surgery to review your food intake. Your first post-operative clinic visit with the dietitian will be at 3 to 6 weeks following surgery and then monthly for the first 6 months, and every 3 to 6 months for the first two years.



















